 National Rural Health Commissioner: Putting the rural health agenda back on track Dr Ayman Shenouda A rural champion A visit this week to Wagga from our National Rural Health Commissioner Professor Paul Worley provided a great chance to work through some of our highest rural health priorities. This new champion for rural patients is exactly what we needed. He fits the job description well – independent, impartial and “a fearless champion” for rural health. He also has alongside him a strong rural health sector full of ideas for building a strong Australian rural health system. Getting the agenda back on track Rural patients are finally getting the focus they deserve and this is our chance to get the rural health agenda back on track. I think we finally have the policy settings in place for this to occur. But it all has to be orchestrated in a way that sees very specific locational needs acknowledged and addressed. This is where the new rural commissioner role comes in. We all have a key role here. There’s still a great deal of work which now needs to occur to ensure every instrument in this vital ensemble can be fully utilised. It is those featured instruments – whether string, woodwind, brass or percussion – each with its own unique qualities that really need to shine. These are the ones that fill in a critical gap and vital if we are going to provide a performance worthy of rural Australians. National Rural Generalist Pathway The first task is the National Rural Generalist Pathway. If we are to get this policy right we will need a broad policy lens with a commitment to needs-based planning encompassing all disciplines. We know that a sustainable health workforce solution for rural Australia needs to factor in flexibility in policy design. By this, I mean allowing for an optimal skill mix which is capable of meeting the very specific service needs of that community. Local needs analysis It is clear that we need reforms that can address maldistribution to meet growing service demand. But to do this we need to look at what is really happening in these communities. Skills planning through a rural generalist pathway solution must, therefore, encompass a much broader skill mapping exercise. This needs to be steered toward more integrated care and with a focus on the full multidisciplinary skill mix required to keep those services going. We need to find ways to capture current skill depth so that this can be prioritised better in policy. Reinforcing the importance of primary care and coordination of care so that the policies can follow. But really plotting that essential skill mix required to support rural models of care. Future supply and demand (against need) It is about having that critical mass of health professionals to achieve a sustainable service environment. This not only lifts constraints enabling more equitable access to services but creates a way to mobilise and build on peer support. In turn, reducing burn-out by formalising mechanisms for peer support-support networks. It provides safer working hours and leaves room for internal backfill for relief, as well as professional development or space to take on a supervising role. There’s been plenty of workforce planning occurring – PHNs, LHNs, and RHWAs – but we lack that common formula. No-one can see at a national level where the true hotspots are. We need to establish what constitutes a minimum workforce requirement or mix for a particular population size and then apply that across the country. Matching and forecasting the needs is complex but we have evidence-based approaches to estimating health workforce demand. HWA did years of work around it. I think we must clarify this area of workforce policy as a first key step. Once we have this formula then we’ll see a situation where training investment meets demand. There is just not enough aligning in terms of training pathways with workforce planning. This is vital as you can’t have a situation where you have three GP anaesthetists and no GP-obstetrician. This level of planning would also help in terms of succession planning and reassure those committing to these pathways that there is or will be a position for them. It provides a planned career pathway for them. Broad skill depth Broad skill depth is vital to addressing patient need in rural communities. We need to find a way to embed in workforce policy those skills most relied on in meeting this need. I think the discussion is also broader than the training pathway itself. We have to have an equal focus on the requirements of the existing workforce in meeting shifting community need. Training solutions need to enable private community-based practice. We really need to ensure we encompass a range of approaches factoring both procedural and non-procedural skills if we are going to align closely to need. If we support the full skillset required then we are closer to reflecting within the training the full scope of skills practised in rural general practice to meet community needs. This is how we can ensure we produce the next generation of doctors with the skills needed to provide both primary and secondary care. Training Hubs Past policies have had an impact on both recruitment and retention. It all comes back to securing that critical mass (of students). Early exposure which can establish that community connection early which can continue through to intern, prevocational and vocational training years. We’ve always said that we need to invest in more localised training solutions to provide for that community connection and rebuild a teaching culture. The hubs are well positioned to facilitate that vital community connection and link the various stages of training in a rural setting across the full training continuum. The training hubs provide that essential framework now but it is about facilitating those vital partnerships. This is how we can structure training against local healthcare need and service construct and build in those supportive factors so early exposure can be a positive experience. Nurture rural intention We need to nurture rural intention through targeted incentives and sufficient rural exposure strategies. A strong commitment to rural should come with benefits. Capture those wanting to pursue rural through a nurtured pathway and supports which include an investment in mentoring. Truly support RMOs skills and career path aspirations and reinvesting in these years by getting back the PGPPP in its true form. Newly developed policy offering primary care rotations through the new rural community-based interns is certainly acknowledged but it is a minimised model which really needs to be expanded. Vertical continuity over time Focusing more effort on areas that provide both a training benefit and meet a community health need is a way to secure an enduring rural benefit. Realising that a focus on the full multidisciplinary team is key to providing more integrated and improved patient-care strategies. Building this capacity through vertical integration of teaching and learning which promotes shared responsibilities. It’s that continuity that is needed most – vertical continuity over time to allow for varied exposure which results in the more resilient doctor. Flexibility is needed to ensure training reflects the local service context with an equal focus on community-based training. It helps develop that understanding of optimal care pathways providing continuity of care and a collaborative integrated care approach. Team and teaching culture Developing a strong team culture early has to also be a key focus. Those working in rural Australia know that it takes a dedicated team and an enduring local commitment to tackling the many challenges in delivering regional, rural and remote healthcare. We need to ensure more exposure to multidisciplinary team environments as well as enabling hospital and community partnerships through supportive policy. This is where the pathway solution has to extend beyond a focus solely on medicine. Improved support for supervisors has never had the policy focus it deserves. We need to increase the teaching capacity of rural communities while minimising the impact of burnout. Practice viability is a major consideration here. All these factors need to be considered in terms of ensuring a rural GP can take on a training or teaching role. Succession planning and providing that easy entry, gracious exit is key and would lift the load for many already overcommitted. A more sustainable future In designing rural policies which can provide a more sustainable future, the focus clearly has to come back to addressing health disparities between rural and urban Australians. A resilient multi-skilled generalist workforce capable of meeting current patient need now and into the future is all part of meeting that key requirement. We really need to capitalise on the policy settings we already have in place. The strong planning role of the PHNs and LHNs in identifying local level need. The facilitation role of the new training hubs in ensuring a more positive rural training experience. Existing strong College pathways and well-developed rural skills training program with inter-professional partnerships to build from. We now have that vital role in the National Rural Health Commissioner to ensure a more coordinated national policy and planning effort can occur. We’re well on our way in putting the rural health agenda back on track ensuring lasting change for rural Australians. [ends] Source: RACGP 2014. New approaches to integrated rural training for medical practitioners. Final Report. Available at: https://www.racgp.org.au/download/Documents/Rural/nrffinalreport.pdf
0 Comments
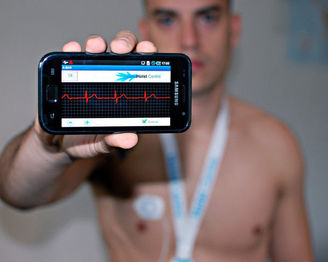 A digital health future: The risks and opportunities Dr Ayman Shenouda An uncertain future Technology will never replace doctors. That part is clear (or to me at least). But there’s still a lot of uncertainty ahead and we’re all being told to prepare for significant changes. We’re now seeing daily discussions around the Fourth Industrial Revolution and that it will see unprecedented workforce change. Despite threats of robot doctors, online lawyers and automated architects, it will be those distinctly human capabilities that will prevail. It is our heart that distinguishes here and no amount of automation can replace it.[1] At the same time, we will need to be ready for it. Because, if, as predicted, technology sees radically different healthcare systems emerge we need to be ready to embrace this change. Leadership will be required in shaping and refining quality standards to ensure continued best care for our patients. Change is already here There are already some significant advances taking place providing a glimpse of what is to come. Much of what we are seeing now is user-driven as technology uptake in the community increases such as through iPhone health monitoring apps. There is certain strength in technology in empowering patients to take responsibility for their own health. Many aim to support self-management outcomes through patient empowerment, but it is clear that a lack of evidence-base undermines quality and safety in some. There is discussion around how certain free medical apps are placing patients at risk through false or misleading claims. From instant blood pressure apps giving falsely normal values to apps that claim to measure blood pressure, oxygenation, and more – all without any peripherals.[2] Health apps present significant challenges to regulatory authorities. And I’m sure it’s not easy for developers to navigate the regulatory pathways either. In Australia, we have TGA guidelines for what software constitutes a medical device. But how much monitoring is being undertaken to identify non-compliance, particularly around claims on these apps, is unclear. The next phase of change It’s clear a soulless search engine or app device is a long way from replacing a GP. But what about the next phase of change? Deep learning breakthroughs of machine learning and artificial intelligence and precision medicine are likely to influence the way we provide care. Big data analytics involve descriptive analytics, predictive analytics, and prescriptive analytics. It is the latter, in prescriptive analytics, which leverages descriptive reports and predictive data to identify actions that would produce maximum value to help us develop and adhere to optimal clinical pathways.[3] Clinical decision support (CDS) on the other hand is set to enhance health and healthcare teams. It will provide both healthcare teams and individuals with knowledge and person-specific information, intelligently filtered or presented at appropriate times, to enhance health and healthcare. CDS encompasses a variety of tools to enhance decision-making in the clinical workflow.[4] GP leadership If the future of medicine is based on data and analytics in guiding decision making, then most critical to success will be that the GP remains in control of the clinical decision-making. To safeguard patients, address questions of liability, and foster trust we need transparency in terms of how clinical decision support tools derive their results.[5] Developers and vendors of clinical decision support tools must be transparent about their methodologies, capabilities, data sources, and limitations.[6] CDS in developing treatment plans will require leadership from the profession in terms of how we can integrate these systems successfully into our practices. In testing the efficacy of these emerging technology in improving the care and treatment of patients there will be a need for strong consistent discipline specific input. For Australian general practice, there is a role for our College in joining multidisciplinary technology assessment committees. Currently, the RACGP Expert Committee – eHealth and Practice Systems lead much of this work. The RACGP Technology Survey released earlier this month will help to gain more insight into the current trends in technology adoption in general practice.[7] It will be interesting to see these results (which closed 3 December) particularly the views of technology use to improve collection of patient data and for clinical decision making. Benefits in service improvements Emergent technologies which present new opportunities for healthcare service provision provide great promise. These are technologies that interface with patients in maintaining health, receiving care, and managing a condition. These new types of technologies – wearables, ingestibles, and embeddables – will be transformative. Management in the home for the elderly and frail will benefit significantly from new technical innovations. Just by adding in a number of sensors to the body to monitor we will support older Australian’s independence as well as take some pressures off the service system while keeping them safe. Reliance on these systems would need to be balanced or potentially worsen social isolation and loneliness which are already significant health risks for the elderly. The value of human contact and continued doctor-patient and nurse-patient relationships are vital here. Wearable technology The next phase of wearable technologies will see patients constantly monitored remotely through wearable skins sensors or smartphone apps with data uploaded directly to their health record.[8] These technologies aim to support the management of chronic diseases, such as diabetes and heart disease. The advent of the digital health coach (Next IT) to remind patients to take medications, schedule doctor appointments represent a new type of technology to support medication adherence. The UK is leading the wearable technology space with pilots underway which will see patients’ issues with state of the art wearable technology. These initiatives are designed to take pressure off the system but also to monitor conditions more effectively for a diverse patient cohort. Some pilots will enable independence for the aged through home monitoring systems with others supporting mental health patients stay in touch with support networks.[9] It is predicted that, as part of a widespread digital revolution of healthcare in Britain, within 5 years patients across the country will go online to speak to their GP via video link, order prescriptions or see their entire health record.[10] Digital divide For implementation in Australia, a final note on the digital divide is warranted. Equity remains an issue despite the promises of high patient engagement through new technologies. So much of the discussion around technology as an access enabler really misses this point. What about those millions of Australian households living without an internet connection? Telehealth implementation has been patchy in rural Australia due to the lack of fast and reliable internet, despite the (slow) rollout of NBN. Assuming we all get access by the time these technologies are fully realised, not all Australians can afford access to the internet or the digital resources required to drive new innovations. For equitable access, we would need to see policies that can provide unmetered online access for the disadvantaged. A commitment to extend the Health Care Card to address the digital divide should be in the planning if we are to strive for equitable access outcomes. Leading the discussion Healthcare’s technology revolution is likely to see significant change. Doctors have been described as late adopters of technology in the past. It will be important to be ready and even more important to be part of the discussion. That is, the one that is occurring now! Finding new ways to connect patients to our practice is positive and possible right now. Future broader technology enabled supports to integrate services and strengthen monitoring of patients can see a positive new change which can only enrich patient care. We’re on the cusp of enormous change and our combined leadership is required in balancing risk with opportunity. Let’s all take up the challenge. End [1] PwC. 20th CEO Survey. The talent challenge: Harnessing the power of human skills in the machine age. PwC. 2017. Available at: https://www.pwc.com/gx/en/ceo-survey/2017/deep-dives/ceo-survey-global-talent.pdf [2] Misra, S. IMedicalApps Feature. Another top free medical app that puts patients at risk with claims to measure blood pressure, oxygenation, and more. 26 October 2016. Available at: https://www.imedicalapps.com/2016/10/icare-health-monitor-health-app-patient-risk/ [3] Bresnick J. HealthIT Analytics Feature. The Difference Between Clinical Decision Support, Big Data Analytics. 31 August 2017. Available at: https://healthitanalytics.com/news/the-difference-between-clinical-decision-support-big-data-analytics [4] Ibid. [5] Bresnick J. HealthIT Analytics Feature. Transparency is key for clinical decision support, machine learning tools. 6 September 2017. https://healthitanalytics.com/news/transparency-is-key-for-clinical-decision-support-machine-learning-vendors [6] Ibid. [7] RACGP. Webpage. RACGP Technology Survey 2017. Available at: https://www.racgp.org.au/your-practice/ehealth/additional-resources/racgp-technology-survey/ [8] Skokowski P. Wearable Tech Feature. Wear your health on your sleeve: The next phase of wearable technology. 25 September 2015. Available at: http://www.wearabletechnology-news.com/news/2015/sep/25/wear-your-health-your-sleeve-next-phase-wearable-technology/ [9] Knapton S. The Telegraph. NHS remote monitoring will allow dementia patients to stay at home. 22 January 2016. Available at: http://www.telegraph.co.uk/news/health/elder/12113536/NHS-remote-monitoring-will-allow-dementia-patients-to-stay-at-home.html [10] Rigby M. Digital Health London. Spotlight: Innovation and Integration – The Future of General Practice. Available at: https://digitalhealth.london/spotlight-innovation-integration-future-general-practice/  Dr Ayman Shenouda Shaping Australia: one GP at a time For those who attended GP17 in October, I’m sure you will agree that it was delivered to its usual high standard and there was plenty of diversity in terms of viewpoints. Some perspectives were what could only be described as poles apart. Dr Jay Parkinson and Sir Harry Burns for example. Dr Parkinson with his discussion around consulting in the cloud through to Sir Harry’s on tackling poverty. There have been some blogs and articles around the technology discussion including recent Opinion in the Medical Observer. It was Sir Harry’s discussion that moved me the most as he provided some important insights into poverty and particularly around social chaos and its flow-on effects in eroding wellness. In some ways, this discussion gave me renewed hope. That as a community we can together tackle disadvantage particularly in ensuring our children get the best start in life. Not enough wellness Sir Harry Burns from Strathclyde University and former Chief Medical Officer for Scotland provided the research keynote address. This was a spirited defence of poverty which really got to the heart of the issue. The issue, of course, being disparities in terms of health outcomes and ways to counter these. It’s about how societies can create wellness and also how they can destroy it. In explaining this, he brings the consequences of poverty and inequity into sharp focus. His own country’s poor health, he says, is a reflection only of the health of the poor. Studies he’d undertaken led him to believe that the problem was in fact not enough wellness (and not too much illness). Social conditions as fundamental causes of health could be seen through countless studies he shared. We’ve all seen this of course in our own communities. I know in Wagga like most regional towns there are some deeply entrenched social disparities. But in addressing these, our national policy I think is structured in a way to deal with consequences, not poverty prevention and reduction. And without significant change, these patterns will only continue. The science behind wellness Sir Harry’s work has sought to unravel the science behind wellness. And I think some of the key learnings from his research can really transform our policies here in Australia today. It was the work of a colleague, Professor Alastair Leyland, which examined his own community of Glasgow against the slope index of inequality, which began his own inquiry around what causes health inequalities. Some very specific insights were shown in terms of what happened in society to slow down growth and life expectancy in the poor. The peak in mortality shown in these studies was in the young – teenage and young working age people – and from very specific causes – drugs, alcohol, suicide, and violence. Inequality mortality was not a feature of the elderly. These were not people dying from heart disease or cancer but there was something else going on in the population. These outcomes were pyschosoically determined - society determined causes of premature death - and they needed to work out what the key drivers were. It was social chaos that intervened which came with the housing disruption more than five decades ago. Traditional communities were broken as a consequence alongside loss of employment, opportunity, and hope. This was what eroded wellness and it is clear the same social disruption occurred here and we are also dealing with these same issues. Causes of wellness Looking more to those causes of wellness. Salutogenesis and the work of an American Sociology Dr Anton Antonovsky around a Sense of Coherence which relies on a life which is structured, predictable, explainable. Having resilience or the internal resources and will to deal with challenges. In quoting Antonovsky he said: “Unless you can see the world as comprehensible, manageable and meaningful you will experience a state of chronic stress.” This provided what he was looking for. It showed the link between social circumstances and ill health. Poverty and elevated stress The research presented really showed the relationship between poverty and elevated stress and how that leads to chronic disease and ill health. Those with a difficult start are less equipped to adapt to change which often manifests in poor behaviours. Studies by Bruce McEwen of Rockefeller University has made those links as well as Sir Harry’s own associated work undertaken in Glasgow. Early-life stress and the long-lasting behavioural, mental and physical consequences. For those wanting to learn the full science behind this here is his presentation and this discussion is about 20 minutes in. And there’s something in a cuddle. The molecular biology of a cuddle was shown. Comforting and its effect on suppressing the stress response. The biochemical toll of early neglect. Stress in infancy and the fact that neglected babies don’t get enough 5-HT. The work of Michael Meaney’s and the difference in brain development for those children who experience adversity in early life was shown. Other studies were shown which have looked at different types of adverse childhood events – neglect, abuse, domestic violence, alcoholic parent – which is then linked to outcome. It showed children exposed to adverse events in early life had a higher risk of alcoholism, depression or drug abuse. Breaking the cycle Social turbulence was the description used. More specifically, he described a cycle that alienates people and impairs their ability to control their wellbeing. And that it starts with chaotic early years. The policy learnings for us include around Scotland’s approach to improving wellness. That is to focus on breaking that cycle by doing things in early life. Policy solutions There are some key learnings in the policy approach itself. It was those at the front-line who developed the policy solutions in Scotland in response to these issues. They asked front-line staff for solutions, then took their ideas and tested them and shared them across the country. The secret, he says, is in marginal gains. Go out there try lots of things see what works and then do it all consistency. I think there’s a lesson in that for our own policy development. It is through those small gains which from a range of interventions that add up to produce significant overall improvements. In early years, it was simple things like attachment is improved if kids are read bedtime stories. The solution lies in enabling that to occur. Policy approach The shift in policy approach is really about enabling policy change. That is change as opposed to full reform. It is in enabling those incremental shifts to existing structures, or the adoption of new and innovative approaches that can facilitate that change. The risk in full reform is that it stifles innovation which can limit participation and if it’s not realised quickly then all is lost including those approaches that proved to work. Politicians turn to the next new thing which may not be as effective. In Scotland, they’ve had 1500 small tests of change carried out in child health with 60 or 70 of them now implemented. Similar community strengthening type approaches which can facilitate incremental gains are what we need here to shift disparities. Conclusion The key message from the discussion is that it is those experiences in early life which can set off a life course of adversity. Those clear links in social circumstances and the beginnings of chronic ill health. We need much more focus here in Australia on what causes wellness. It’s not that we haven’t had a focus here on concepts which include community resilience. Those social capital discussions were full of it in the early 2000s. There seems less focus now and perhaps its due to governments not realising fully how investments now pay health dividends later on. There also may not be that political will to invest in wellness knowing the results will not be seen in the space of an electoral term. |
Author
Dr Ayman Shenouda Blogs categories
All
|
